Insights on Quality, Risk, Governance, and Emerging Technology
Quality & Compliance
• Compliance Architecture
• Audit Strategy
• Regulatory Readiness
• Operational Discipline
Risk & Governance
• Governance
• Risk Intelligence
• Executive Oversight
• Cyber Resilience
Innovation & Systems
• AI Accountability
• Structured Innovation
• Systems Thinking
Welcome to the Insights section of Systemic Quality Consulting.
Here we explore the intersection of quality systems, regulatory compliance, risk governance, and emerging technologies such as artificial intelligence. Our goal is to provide practical perspectives that help organizations build systems that perform under scrutiny.
Quality leads to Compliance.
Compliance reveals Risk.
Risk demands Governance.
Governance drives Performance.
Performance produces Insight.
Insight creates Systemic improvement.
Cyber risk in healthcare is no longer limited to protecting a single EHR system.
As hospitals migrate from Cerner to Epic, integrate laboratory and radiology systems, adopt cloud platforms, and begin using AI tools, every new integration point creates another potential pathway for cyber threats, data leakage, or operational disruption.
Healthcare remains one of the most targeted industries because patient data is extremely valuable. Modern healthcare environments often include:
• EHR systems
• Laboratory Information Systems (LIS)
• Radiology Information Systems (RIS)
• Cloud vendors
• Telehealth platforms
• AI-enabled documentation and analytics tools
During migrations and integrations, organizations face risks such as:
• insecure data transfers
• poorly controlled temporary storage
• excessive vendor access
• weak audit logging
• outdated systems remaining active during transition
One of the biggest risks is third-party exposure. A hospital may have strong internal security, but if a connected vendor, cloud provider, or AI platform has weak controls, the organization still inherits that risk.
AI introduces an additional layer of concern.
Healthcare organizations are increasingly using AI for:
• documentation support
• coding and billing
• imaging review
• predictive analytics
• workflow automation
But many organizations still do not have formal AI governance programs in place.
Without proper controls, AI can introduce:
• unauthorized sharing of protected health information
• inaccurate or biased outputs
• lack of transparency in clinical decisions
• insufficient monitoring of how patient data is used
This is why governance is becoming just as important as cybersecurity.
Healthcare organizations need clear answers to questions such as:
• Who owns the data?
• Who can access it?
• How are vendors approved and monitored?
• How are AI tools reviewed before use?
• What happens if a vendor experiences a breach?
Strong frameworks such as HIPAA, the NIST Cybersecurity Framework, and the NIST AI Risk Management Framework can help organizations strengthen controls around healthcare data, AI adoption, vendor oversight, and incident response.
Cybersecurity, AI, and governance can no longer be treated as separate initiatives.
The organizations that will be most successful are those that integrate governance, risk management, and audit readiness into every healthcare technology project from the beginning — not after a problem occurs.


Why EHR Implementations and Transitions Often Struggle — And It’s Not the Technology
After working across clinical and laboratory environments, one thing has become clear to me: Most healthcare organizations don’t struggle with EHR systems because of the technology itself. They struggle because of workflow misalignment. Whether it’s a new implementation or a transition (Cerner → Epic, Meditech → Epic, etc.), the same patterns show up:
• workflows are not fully mapped before Go-live
• training focuses on system navigation rather than clinical processes
• configurations are built without a deep understanding of real patient flow
The result is predictable:
→ increased documentation burden
→ frustrated physicians and staff
→ reduced operational efficiency
→ slower patient throughput
EHR transitions, in particular, are often underestimated. They are not just data migration projects — they are full clinical transformation efforts that require:
• workflow redesign
• cross-department coordination
• integration with systems like LIS and RIS
• structured change management
Without that level of planning, organizations often see a drop in productivity after Go-live instead of improvement. Another common misconception is treating workflow issues as purely technical problems.
In reality, most inefficiencies come from:
• process design gaps
• misalignment between clinical practice and system configuration
• lack of communication between IT and clinical teams
Technology should support clinical care — not dictate it. This is where clinical informatics plays a critical role. Bridging the gap between clinical operations and system design is what ultimately determines whether an implementation succeeds or struggles.
The organizations that get it right focus on one principle: “Clinical workflow first. System second.”

Most people still think EMRs are just where doctors document patient visits. That’s outdated. Today, platforms like Epic, Oracle Health Cerner, and MEDITECH are evolving into central command systems for healthcare operations.
And three major shifts are driving that transformation.
Integration is now the backbone of healthcare. Systems no longer operate in silos. Everything is connected—EHR to lab systems, imaging, and external providers. Behind the scenes, this is powered by standards like HL7 and FHIR, along with integration engines such as Mirth Connect and Cloverleaf Integration Suite. The real challenge today is not just moving data, but ensuring that data is accurate, consistent, and clinically meaningful across systems.
Modernization is replacing fragmentation. Hospitals are moving away from disconnected systems toward fully integrated platforms. We are seeing migration to unified EHR ecosystems, replacement of legacy systems, and a stronger focus on data governance, auditability, and compliance. Bad data in healthcare is not just an IT issue—it is a patient safety issue.
AI is quietly changing everything. It is no longer a future concept in healthcare—it is already embedded in workflows. From clinical decision support to automated documentation and predictive analytics, AI is transforming how care is delivered. But AI is only as good as the data and systems behind it. Integration, data validation, and governance are now more important than ever.
The new competitive advantage in healthcare IT is not just technical skill or clinical knowledge alone. It is the ability to bridge clinical workflows, system integration, data quality, and compliance. EMRs are evolving into intelligent, interconnected ecosystems. The real opportunity is not just using them, but understanding how they connect, how data flows, and how to make them work better together.
Curious—what trends are you seeing in your organization?

Artificial Intelligence and the Future of Professional Work
How AI Is Transforming Law, Medicine, and Knowledge-Based Professions
Artificial Intelligence (AI) has rapidly evolved from a niche technology used primarily by research laboratories and large technology companies into a widely adopted professional tool across nearly every industry. In recent years, the emergence of generative AI systems—capable of analyzing large datasets, generating text, summarizing complex information, and assisting with decision-making—has accelerated its integration into daily professional work.
Today, AI is no longer an experimental technology. It is increasingly becoming an operational layer embedded into professional workflows in industries such as healthcare, law, finance, consulting, and education. The question facing many professionals is no longer “Will AI affect my profession?” but rather “To what extent will AI reshape how my profession operates?”
The Rapid Adoption of AI in Professional Services
Several studies show that AI adoption in professional environments has increased dramatically in the last few years.
According to global labor market analyses, generative AI could automate tasks representing approximately 25% of work hours in the United States, particularly in knowledge-based professions that rely on information processing, writing, and analysis.
Similarly, research from McKinsey suggests that by 2030, roughly 30% of current work activities in the U.S. economy could be automated, significantly altering how professionals perform their jobs.
Despite these disruptive projections, most experts agree that the impact of AI will not simply be job elimination. Instead, it will be job transformation, where technology augments professional capabilities rather than completely replacing human expertise.
AI in the Legal Profession
The legal field provides one of the clearest examples of how AI is transforming professional work.
Historically, legal practice involved extensive manual research, document review, contract analysis, and case law interpretation. These tasks are highly structured and data-intensive making them particularly well suited for AI-assisted automation.
Recent research indicates that AI adoption among legal professionals has increased dramatically, with approximately 69% of legal practitioners reporting the use of generative AI tools in their work.
In addition, labor studies estimate that approximately 44% of tasks within the legal profession could potentially be automated or significantly augmented by AI technologies.
Examples of current AI applications in legal practice include:
Legal research automation
Contract analysis and risk detection
Case law summation
Litigation prediction models
Document drafting assistance
However, while AI can assist with information processing, it cannot easily replicate essential legal functions such as strategic judgment, negotiation, ethical interpretation, and courtroom advocacy.
As a result, the most likely outcome is not the replacement of lawyers, but the emergence of AI-augmented legal professionals who can analyze more cases, produce faster research, and deliver higher efficiency.
AI in Healthcare and Medical Practice
Healthcare is another field experiencing rapid AI integration, though the impact differs from that of the legal sector.
A survey conducted by the American Medical Association found that 66% of physicians reported using some form of AI in their practice by 2024, up significantly from only 38% the year before.
AI applications in healthcare currently include:
Medical imaging analysis
Diagnostic assistance
Patient triage systems
Clinical documentation automation
Predictive analytics for disease management
In certain specialties such as radiology, AI has demonstrated the ability to detect patterns in imaging data faster than human clinicians. However, even in these fields, AI functions primarily as a decision-support system rather than an autonomous practitioner.
Healthcare remains particularly resistant to full automation due to several factors:
Regulatory oversight
Ethical accountability
Need for human empathy and communication
Complex diagnostic reasoning
Studies among physicians suggest that while AI may replace administrative and documentation tasks, very few clinicians believe AI will fully replace physicians in delivering patient care.
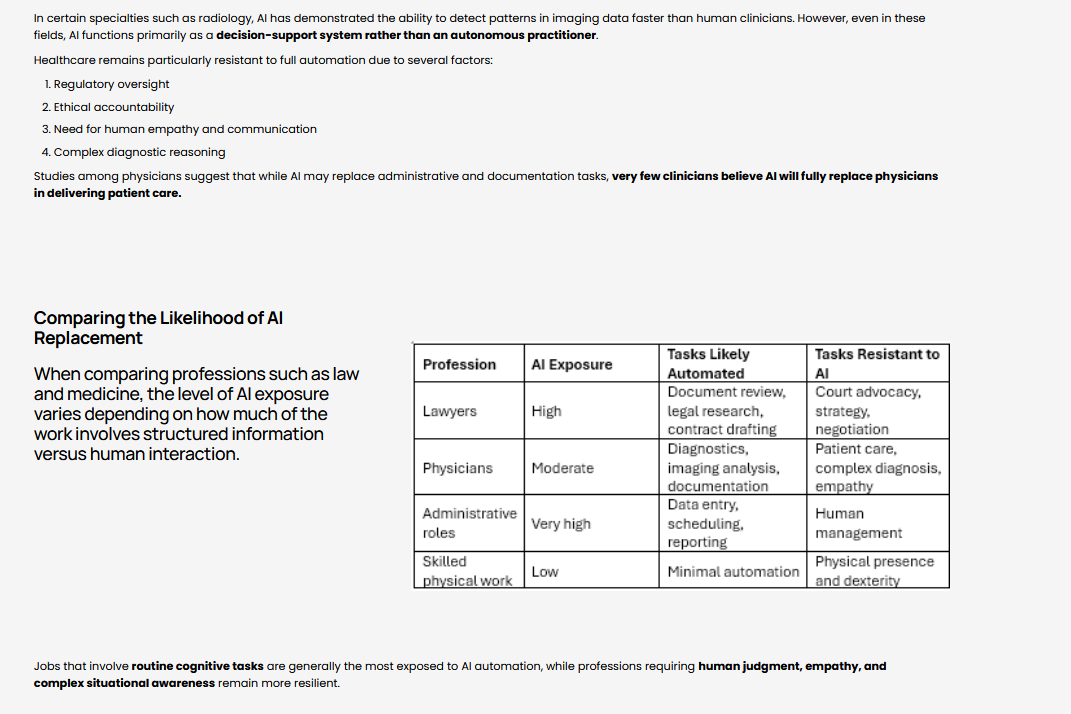
Comparing the Likelihood of AI Replacement
When comparing professions such as law and medicine, the level of AI exposure varies depending on how much of the work involves structured information versus human interaction.
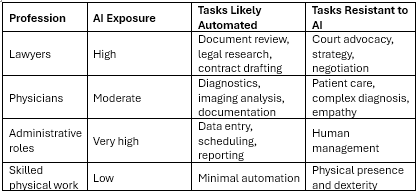
Jobs that involve routine cognitive tasks are generally the most exposed to AI automation, while professions requiring human judgment, empathy, and complex situational awareness remain more resilient.
Global Workforce Impact and Projections
Major economic institutions have published striking projections regarding the long-term impact of AI on employment.
A report from Goldman Sachs estimated that AI could affect the equivalent of 300 million full-time jobs worldwide, primarily by automating certain tasks within those roles rather than eliminating entire professions.
Other economic forecasts suggest:
8% of global jobs may be displaced by 2030, while many new technology-related roles will emerge.
AI could increase global productivity significantly, potentially contributing trillions of dollars to economic output over the next decade.
The transformation will therefore involve both disruption and opportunity.
The Future: Human-AI Collaboration
Rather than replacing professionals outright, AI is likely to redefine professional expertise.
Lawyers may increasingly rely on AI-powered research platforms to process thousands of cases instantly. Physicians may use AI-assisted diagnostics to detect diseases earlier than ever before. Consultants and analysts may use predictive models to evaluate risks and opportunities at unprecedented scale.
The emerging model is not human vs. machine, but human with machine.
Professionals who learn to leverage AI tools effectively will likely become significantly more productive than those who do not.
Conclusion
Artificial Intelligence is already transforming the professional landscape across law, medicine, and many other knowledge-based industries. While AI will automate certain routine tasks, the most critical aspects of professional work—judgment, ethics, creativity, and human interaction—remain deeply human.
For organizations and professionals alike, the strategic challenge is not resisting AI adoption but learning how to integrate AI responsibly, efficiently, and ethically into existing professional frameworks.
Those who successfully adapt will not be replaced by AI—they will be empowered by it.
Author:
Joseph (Joe) Shiferaw
Founder & Principal Consultant
Systemic Quality Consulting LLC
Specializing in quality systems, regulatory compliance, and audit-ready operational frameworks across healthcare, technology, and regulated industries.

Most AI Risk Is Not Technical. It’s Governance Failure
Boards are asking about AI strategy. Very few are asking about AI control architecture. That’s the gap. AI is now generating policies, influencing decisions, supporting clinical judgments, shaping underwriting models, and drafting regulatory documentation. Yet in many organizations AI outputs are not mapped to risk registers, AI-assisted decisions lack traceability standards, Internal audit plans do not include AI process testing, Executive accountability for AI oversight is undefined and Incident response frameworks ignore AI-generated error exposure
The coming shift will not be about better models. It will be about demonstrable oversight. Expect near-term movement toward: Formal AI accountability at the executive level, Audit scrutiny of AI-assisted documentation, Regulatory guidance on explainability and validation, Convergence between AI governance, cyber risk, and enterprise risk management and Insurance underwriting tied to AI control maturity.
AI is no longer experimentation. It is becoming regulated infrastructure. Organizations that treat AI as a tool will face friction. Organizations that treat AI as a governance domain will build resilience. The real question is not whether you use AI. It’s whether you can defend it under scrutiny.



Environment Influences Performance —
And Most Leaders Overlook It
Most organizations invest heavily in systems, technology, and talent.
Yet very few organizations intentionally design the visual environment where those systems operate. And environment influences performance.
In professional settings — visual structure affects clarity, focus, emotional regulation, and decision-making tone. Research in workplace psychology and environmental design consistently demonstrates that surroundings influence stress levels, cognitive fatigue, engagement, and perceived stability.
We audit systems.
But we rarely audit space.
Art in professional environments is often misunderstood as decoration — an aesthetic afterthought. When thoughtfully selected and strategically placed, it becomes something far more consequential: environmental architecture.
Large-scale anchor installations in leadership spaces establish presence and intellectual depth. They signal intention. They shape tone before a word is spoken in a boardroom. In executive offices, structured contemporary works reinforce clarity and authority without distraction.
In healthcare settings, the stakes are even higher.
Clinical and laboratory environments operate under sustained cognitive pressure. Staff manage regulation, documentation, patient vulnerability, and technical precision daily. Visual chaos amplifies fatigue. Visual order supports stability.
Structured contemporary work in administrative suites, corridors, waiting areas, and professional offices can reinforce calm without diminishing professionalism. It does not replace compliance, process discipline, or governance — but it complements performance culture.
Rotational art programs introduce controlled renewal. Periodic visual change reduces environmental stagnation and re-energizes professional spaces. Even subtle refresh cycles can influence perception, morale, and cognitive engagement — particularly in environments where teams operate under constant operational demand.
In high-regulation settings, visual order matters. Clean, intentional environments reinforce discipline. Alignment between physical surroundings and organizational mission strengthens institutional identity.
The goal is not decoration.
It is alignment.
Alignment between environment and leadership tone.
Alignment between space and mission.
Alignment between structure and culture.
Through Systemic Quality Studio™, we design corporate art programs for performance-oriented environments — including executive anchor installations, curated rotational programs, commissioned works, and strategic visual consultation tailored to healthcare and professional settings.
Healthcare systems, Compliance systems and Risk frameworks are designed with intention. The spaces surrounding them should be as well.
As executives, we evaluate systems, exposure, and performance indicators.
Perhaps it is time we evaluate the walls, too.

Certification Relevance by Industry: A Risk-Weighted Model
As I expand across healthcare, technology, manufacturing, and government sectors, I evaluate certifications through one lens: Which certification reduces the highest concentration of risk? Rather than ranking by popularity, I built a simplified risk-weighted model.
Scoring Scale
🟥 5 = Critical
🟧 4 = High Strategic
🟨 3 = Operational
🟦 2 = Situational
⬜ 1 = Minimal
Risk factors considered: regulatory exposure, data sensitivity, product safety liability, federal dependency, litigation risk, and market trust.
Risk Snapshot by Industry
Healthcare
ISO 9001 🟨🟨🟨
ISO 27001 🟧🟧🟧🟧
HIPAA 🟥🟥🟥🟥🟥
CAP / CLIA 🟥🟥🟥🟥🟥
Internal Audit 🟥🟥🟥🟥🟥
Primary Risk: regulatory enforcement, PHI exposure, patient safety.
IT / SaaS
ISO 9001 🟨🟨🟨
ISO 27001 🟥🟥🟥🟥🟥
SOC 2 🟥🟥🟥🟥🟥
CMMC 🟧🟧🟧🟧 (federal)
Internal Audit 🟧🟧🟧🟧
Primary Risk: data breach, contractual exposure, vendor risk.
Medical Device Manufacturing
ISO 9001 🟧🟧🟧🟧
ISO 13485 🟥🟥🟥🟥🟥
Internal Audit 🟥🟥🟥🟥🟥
Primary Risk: FDA scrutiny, recall liability, traceability.
Government / Defense
ISO 9001 🟧🟧🟧🟧
ISO 27001 🟧🟧🟧🟧
CMMC 🟥🟥🟥🟥🟥
Internal Audit 🟥🟥🟥🟥🟥
Primary Risk: eligibility, cybersecurity maturity, CUI protection.
Heat View (High Impact Only)
Healthcare
HIPAA █████
CAP/CLIA █████
Internal █████
IT
ISO 27001 █████
SOC 2 █████
Medical Device
ISO 13485 █████
Internal █████
Government
CMMC █████
Internal █████
Cross-Industry Insight
Internal Audit ranks high across every sector. Certifications define structure.
Internal audit validates reality. Healthcare elevates HIPAA. Technology elevates ISO 27001 & SOC. Manufacturing elevates ISO 13485.
Government elevates CMMC.
Maturity appears when these are integrated — not stacked.
Strategic Conclusion:
The real question is not: “What certification should we add?”
It is: “Where is our highest unmanaged risk?”
Certifications are not branding instruments. They are risk-reduction architectures.
ISO 9001 builds discipline.
ISO 27001 protects data.
ISO 13485 protects products.
SOC builds trust.
CMMC enables eligibility.
HIPAA/CAP/CLIA reduce liability.
Internal audit sustains credibility.
The advantage is not accumulation. It is integration.
Joe Shiferaw
Systemic Quality & Compliance Consulting
Building Structured Systems That Actually Work
https://www.linkedin.com/posts/joe-shiferaw-413105316_certification-relevance-by-industry-a-risk-weighted-activity-7429590684413812737-iC67?utm_source=social_share_send&utm_medium=member_desktop_web&rcm=ACoAAFAbEA8Bu4GdbX3pUEdXRs6WMRnLIZqDQlM
Most organizations don’t fail compliance audits because they lack documentation. They fail because they lack discipline. Compliance doesn’t break companies. It exposes them.
It exposes:
• Leadership that doesn’t review performance
• Processes that only exist on paper
• Risks that were never formally assessed
• Corrective actions that were never truly corrective
• Metrics that no one actually uses
You can’t “prepare” your way out of a weak system. Audits are mirrors. And mirrors are uncomfortable when systems are cosmetic. Strong organizations treat compliance as: A management operating system. Weak organizations treat it as: An annual event.
Compliance is not paperwork. It’s structured accountability. And accountability is what most teams avoid.
https://www.linkedin.com/posts/joe-shiferaw-413105316_most-organizations-dont-fail-compliance-activity-7427763491660455937-3v80?utm_source=social_share_send&utm_medium=member_desktop_web&rcm=ACoAAFAbEA8Bu4GdbX3pUEdXRs6WMRnLIZqDQlM


What is frequently underestimated about internal audits includes:
- They are not about finding faults; rather, they reveal system weaknesses early.
- A good audit assesses how processes actually function, not just how procedures are documented.
- Audit results should lead to genuine corrective actions, not merely updates to documentation.
When conducted effectively, internal audits can:
- Reduce surprises during external audits.
- Strengthen management review decisions.
- Improve operational consistency.
- Build confidence across teams.
Internal audits should not be seen as a disruption to the business; they are one of the most effective tools for sustaining compliance and fostering continuous improvement.

There are many consulting companies offering ISO 9001 certification support, but one thing clients quickly discover is that price alone doesn’t tell the full story.
Educated clients usually ask a few key questions before choosing a consultant:
• Which ISO standard are we pursuing? (ISO 9001, ISO 27001, etc.)
• Is the certification body accredited by an IAF- recognized accreditation body?
• How widely accepted is that accreditation — in the U.S. and globally?
• Is pricing flat, or does it scale based on company size, employee count, and scope?
• How long will it realistically take to become audit-ready and compliant?
• Does industry matter? (IT, healthcare, manufacturing, government contracting all carry different expectations.)
One important distinction many organizations miss early on:
👉 Not all ISO certificates are equal.
The accreditation body behind the certification often determines how widely that certificate is accepted by customers, regulators, and partners.
In the U.S., for example, A NAB-accredited certifications are generally the most recognized, particularly in regulated, government-adjacent, and healthcare environments. Other pathways may be appropriate depending on business needs, risk profile, and market.
Another reality:
Most consulting firms don’t publish pricing or accreditation pathways upfront. You usually have to call or email and ask very specific questions to understand what you’re actually paying for — and what level of recognition you’ll receive at the end.
The most successful ISO 9001 efforts I’ve seen are the ones where organizations align accreditation choice, scope, timeline, and industry expectations from the beginning — not after the audit is scheduled.
ISO certification works best when it’s treated as a business decision, not just a checkbox.

Why Most Quality Systems Fail After Certification

Certification is often treated as an endpoint. In reality, it is only a milestone.
Organizations frequently build systems designed to pass an audit — not to sustain operational discipline. Documentation becomes static, ownership becomes unclear, and internal audits lose their strategic function. Over time, the system deteriorates into formality rather than structure.
Sustainable quality systems are embedded into operational workflows. They are led by accountable stakeholders, reviewed with intention, and reinforced through leadership alignment. When systems are treated as living frameworks rather than compliance checklists, they remain resilient long after certification is achieved.
The objective is not to survive audit cycles — but to institutionalize structured performance.
Audit Readiness vs. Audit Survival
There is a meaningful difference between being prepared for an audit and scrambling to survive one.
Audit survival is reactive. It involves last-minute document gathering, inconsistent evidence trails, and temporary corrective actions. It may result in a passing grade, but it rarely produces structural strength.
Audit readiness, by contrast, reflects operational clarity. Documentation is organized, responsibilities are defined, evidence is traceable, and corrective actions are measured for effectiveness — not appearance.
True readiness reduces anxiety, protects leadership credibility, and strengthens long-term governance.
The difference is discipline.
Structure vs. Chaos: What Organizations Can Learn from Systems Thinking
Every organization operates between structure and variability.
Markets shift. Regulations evolve. Personnel change. Risk fluctuates.
Without structured systems, organizations absorb change through friction and confusion. With intentional system design, variability is managed without loss of control.
Systems thinking requires anticipating complexity rather than reacting to it. It involves mapping process inter-dependencies, clarifying accountability, and building documentation that reflects operational reality.
Structure is not rigidity. It is resilience.

Certification is often treated as an endpoint. In reality, it is only a milestone.
Organizations frequently build systems designed to pass an audit — not to sustain operational discipline. Documentation becomes static, ownership becomes unclear, and internal audits lose their strategic function. Over time, the system deteriorates into formality rather than structure.
Sustainable quality systems are embedded into operational workflows. They are led by accountable stakeholders, reviewed with intention, and reinforced through leadership alignment. When systems are treated as living frameworks rather than compliance checklists, they remain resilient long after certification is achieved.
The objective is not to survive audit cycles — but to institutionalize structured performance.

Reactive compliance is expensive.
Reactive compliance is expensive.
When organizations respond to findings only after deficiencies are identified, they accumulate hidden costs: operational disruption, reputational risk, executive distraction, and repeated corrective cycles.
Proactive compliance integrates risk monitoring, internal audit discipline, and structured documentation review before regulators or external auditors intervene.
The investment in structured compliance reduces long-term exposure and strengthens leadership confidence.
Compliance should function as strategic risk management — not crisis response.

The physical environment influences cognitive clarity, focus, and leadership tone.
Executive and professional environments that reflect visual order reinforce disciplined thinking. Structured visual environments support clarity in decision-making and promote consistency in organizational messaging.
Art within corporate spaces should not be decorative alone. It should be intentional — aligned with the identity, structure, and performance expectations of the organization.
Through Systemic Quality Studio™, we extend structured thinking into the physical environment, supporting performance-oriented spaces through curated contemporary art installations.
Environment reinforces culture.
Documentation is not paperwork.
In regulated industries, documentation is organizational memory and legal defense.
Clear version control, traceable approvals, structured CAPA records, and defensible policy frameworks protect organizations during regulatory review and litigation exposure.
When documentation systems are fragmented or informal, risk increases.
Structured documentation is not bureaucratic — it is protective.
Clarity today prevents exposure tomorrow.



Cyber Risk, AI, and Healthcare Data Integration: Why Governance Matters More Than Ever
Healthcare organizations are under increasing pressure to modernize systems, integrate data across departments, and adopt new technologies such as artificial intelligence. Hospitals are migrating from legacy Electronic Health Record (EHR) systems to newer platforms, connecting laboratory, radiology, billing, and clinical systems, and using AI to improve documentation, patient triage, imaging review, and workflow efficiency.
At the same time, cyber risk has become one of the most significant operational threats facing healthcare organizations.
The challenge is no longer simply protecting one EHR system. Modern healthcare environments involve complex ecosystems that include EHR platforms, Laboratory Information Systems (LIS), Radiology Information Systems (RIS), cloud services, vendor platforms, mobile devices, APIs, and AI-enabled tools. Each integration point creates another potential pathway for unauthorized access, ransomware, data leakage, or operational disruption.
Healthcare remains one of the most heavily targeted industries for cyberattacks because healthcare data is highly valuable. Unlike credit card information, patient records contain personal identifiers, insurance data, medical history, billing information, and often Social Security numbers. This makes healthcare organizations prime targets for ransomware groups and cybercriminals. In 2025 alone, at least 642 healthcare data breaches affecting 500 or more individuals were reported, impacting nearly 57 million people.
One of the most significant recent examples was the cyberattack on Change Healthcare, which affected approximately 190 million individuals and disrupted claims processing across the United States. The incident demonstrated how a breach at one technology vendor can impact hospitals, pharmacies, insurers, and patients nationwide.
Key Cybersecurity Risks During Healthcare Data Migration and Integration
1. Weaknesses During EHR Migration
When organizations move from one EHR platform to another, such as from Cerner to Epic or from Meditech to Epic, large volumes of sensitive patient data are extracted, transferred, transformed, and reloaded.
This creates multiple risk points:
insecure data transfer methods
poorly controlled temporary storage locations
incomplete access restrictions during migration
outdated or unpatched systems used during transition
third-party vendor access with excessive permissions
lack of audit logging during conversion processes
Many organizations focus heavily on the technical migration itself but overlook how cyber controls must follow the data throughout the entire process.
2. Increased Third-Party Risk
Healthcare organizations increasingly depend on vendors for cloud hosting, managed services, AI tools, billing platforms, telehealth, laboratory systems, and cybersecurity support.
Every vendor with access to patient data creates additional risk. A hospital may have strong internal controls, but if a connected vendor has weak security practices, the hospital still inherits that risk.
Recent attacks involving healthcare service providers and technology vendors demonstrate that third-party exposure is now one of the largest healthcare cyber risks. Ransomware attacks on healthcare systems increased significantly in 2025, while business associates and vendors remained frequent targets.
3. AI-Related Data Leakage
AI introduces a new layer of cyber and governance risk.
Healthcare organizations are increasingly experimenting with AI for:
clinical documentation assistance
patient communication
coding and billing
predictive analytics
imaging review
operational dashboards
workflow automation
However, AI systems may process sensitive patient information, and many organizations do not yet have formal AI governance programs in place. Research suggests fewer than 25% of enterprises currently maintain mature AI governance frameworks.
Risks include:
unauthorized sharing of protected health information with AI tools
prompt injection attacks
biased or inaccurate outputs
lack of transparency in AI-generated decisions
improper model training using sensitive patient data
insufficient monitoring of AI outputs
over reliance on automated recommendations
Healthcare organizations must recognize that AI systems interacting with Protected Health Information (PHI) require the same level of security, auditability, and access controls as EHR systems. OCR has increasingly emphasized that AI systems processing PHI must maintain access management, audit logging, encryption, vendor risk assessments, workforce training, and minimum necessary data controls.
Why Governance Matters
Cybersecurity alone is not enough. Organizations also need strong governance frameworks to ensure healthcare data is used responsibly, securely, and consistently.
Effective governance helps answer questions such as:
Who owns the data?
Who has access to the data?
What systems are authorized to receive the data?
How are AI tools approved and monitored?
What happens if a vendor experiences a breach?
How are security incidents reported and investigated?
How often are access rights reviewed?
Without governance, even technically secure systems can fail because responsibilities, policies, and oversight are unclear.
Governance Frameworks That Help Reduce Risk
Several frameworks can help healthcare organizations manage cyber risk, AI adoption, and healthcare data integration more effectively.
HIPAA Security Rule
The Office for Civil Rights continues to emphasize risk analysis, system hardening, patch management, access control, and ongoing monitoring as foundational requirements for protecting electronic Protected Health Information (ePHI). OCR audits in 2026 remain heavily focused on Security Rule risk analysis and risk management programs.
NIST Cybersecurity Framework
The National Institute of Standards and Technology Cybersecurity Framework helps organizations identify, protect, detect, respond to, and recover from cyber threats. It is particularly useful for healthcare organizations because it provides structure around risk management, incident response, asset inventories, vendor risk, and security monitoring.
NIST AI Risk Management Framework
The National Institute of Standards and Technology AI Risk Management Framework provides healthcare organizations with a model for governing AI use cases through four functions:
Govern
Map
Measure
Manage
This framework helps organizations address privacy, bias, explainability, accountability, and ongoing monitoring of AI systems. It is designed to work alongside existing cybersecurity and HIPAA programs rather than replace them.
Internal Audits and Vendor Assessments
Healthcare organizations should routinely perform:
HIPAA risk assessments
third-party vendor risk reviews
access control audits
system hardening inspections
penetration testing
AI model reviews
data retention and destruction audits
incident response testing
These audits help organizations identify weak points before they become major incidents.
Moving Forward
Healthcare organizations can no longer treat cybersecurity, AI, and governance as separate initiatives. Data migration, system integration, AI adoption, and cyber risk are now deeply connected.
The organizations that will succeed are those that treat governance as part of every healthcare technology project from the beginning, not as an afterthought after implementation is complete.
Strong governance, regular audits, structured risk analysis, and disciplined vendor oversight are no longer optional. They are essential for protecting patient trust, ensuring compliance, and maintaining resilient healthcare operations in an increasingly connected digital environment.